Computer simulations of the heart have come a long way. In 1993, scientists used PSC’s Cray C90 to make a breakthrough that laid the foundations for today’s cutting-edge simulations.
Early Access on CRAY C90 in 1993 Ironed Out Problems in Early Heart Model

PSC40: Powering Discovery
2026 marks 40 years of PSC. As we continue on with cutting-edge innovation, we look back on four decades of history in computing, education, and groundbreaking research—and the people who made it happen.
In 1993, doctors didn’t have a clear idea of how the mechanics of the heartbeat worked in detail. A computer simulation of the heart in action would give clinicians a tool for testing ideas on how heart disease developed and how they could treat it. Early access to Mario, PSC’s new CRAY C90 supercomputer, allowed a New York University team to fix what had been a problem-plagued computer model of the heart.
WHY IT WAS IMPORTANT

In 1993, as today, heart disease was the number one killer in the U.S. But doctors lacked detailed information on how the healthy heart worked, let alone the diseased one.
Heart disease encompasses a bunch of different ailments, including blocked cardiac arteries that cause heart attacks, weakening of the heart muscles that causes heart failure, and valve disease that can create life-threatening clots. Then as now, doctors wanted to have a better picture of how the heart functions, so they could better understand how diseases derail its function — and how they could step in to repair it.
Charles Peskin and David McQueen of New York University had developed a computer model of the heart. But it wasn’t working. It was kind of a mess; the aortic valve, through which the heart pumps oxygen-rich blood to almost the entire body, wasn’t opening enough to let the normal amount of blood flow through it. Worse, the entire right side of the heart couldn’t eject blood at all.
So much was wrong with the model that they decided to tackle one problem at a time. First, they’d get the aortic valve in their simulation up to speed. To make that happen they turned to Mario, PSC’s third supercomputer, a CRAY C90.

HOW PSC HELPED
Preliminary work on PSC’s second supercomputer, the CRAY Y-MP, had suggested that their simulation just wasn’t detailed enough. Their model, which consisted of a set of points and lines in the computer, would work better if they doubled the number of points contained in each dimension. But doubling a 3D heart would create eight times as many points total, requiring eight times as much computer memory.
The Y-MP, with 512 megabytes of RAM — 16 times less than an iPhone 17 has today — simply couldn’t handle that. The data from the calculations spilled over, slowing the calculations to the point at which just one heartbeat would have taken three years to compute!
Mario, PSC’s new flagship computer, was another story entirely. Sporting what was then a whopping 4,000 megabytes of RAM, or 4 gigabytes, it had (almost) caught up to today’s hot smartphones. At the time, that much memory was huge — enough, the NYU scientists hoped, to get that aortic valve working.
Mario was, as we said, new. So new, in fact, that it wasn’t strictly open for business yet. PSC’s new hot model was undertaking a limited number of projects for expert users to get it all dialed in and tuned up. Peskin and McQueen signed up for such “friendly user” time on the system, helping to get Mario ready for prime time in exchange for early access.
The day came. The team fired up their simulation on the C90, eager to see that aortic valve finally work properly. They got their “three-year” result just days later.
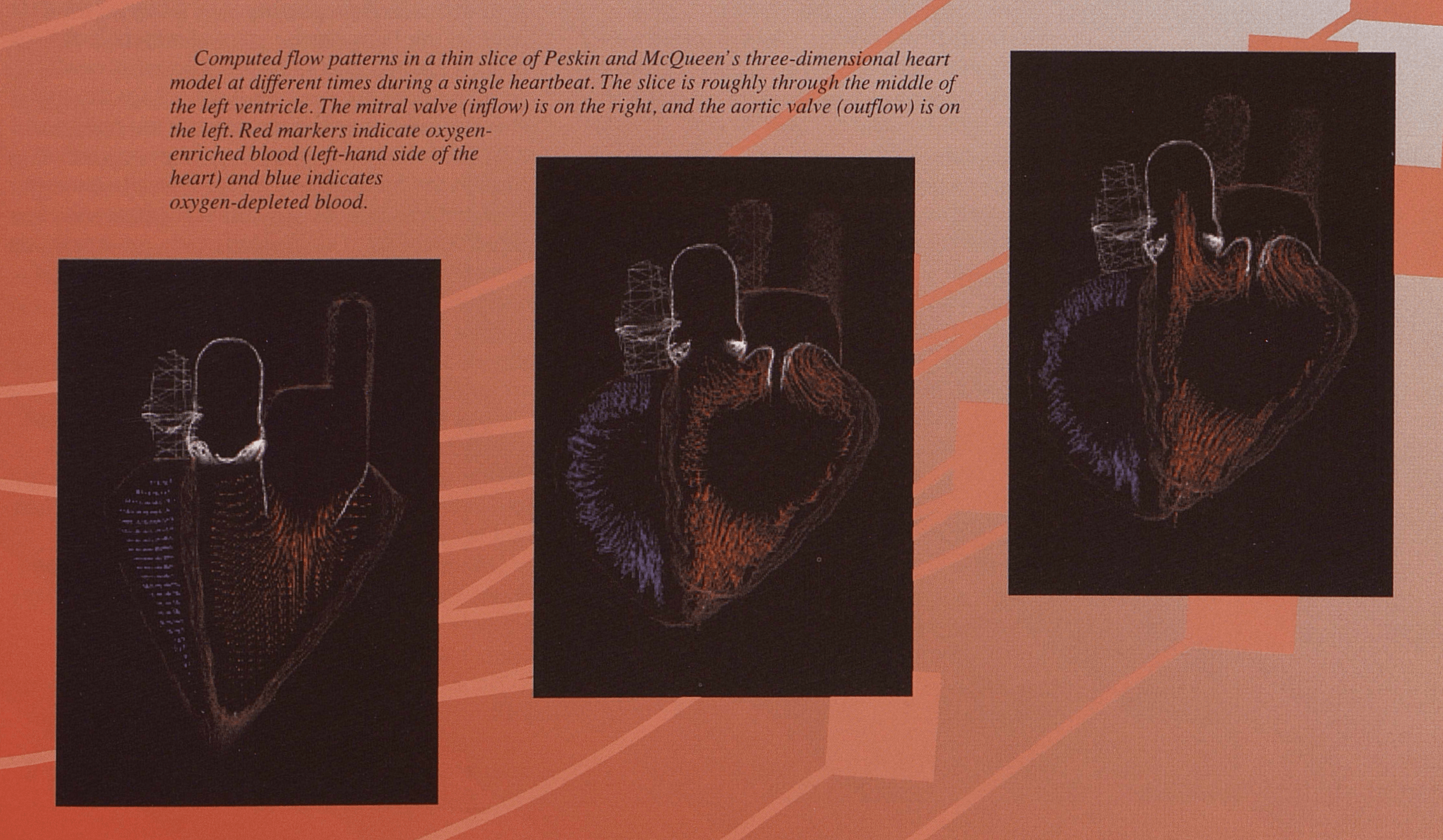
Taken from PSC’s 1993 “Projects in Scientific Computing”: “Computed flow patterns in a thin slice of Peskin and McQueen’s three-dimensional heart model at different times during a single heartbeat. The slice is roughly through he middle of the left ventricle. The mitral valve (inflow) is on the right, and the aortic valve (outflow) is on the left. Red markers indicate oxygen-enriched blood (left-hand side of the heart) and blue indicates oxygen-depleted blood.”

They saw a working aortic valve. But that’s not all. The whole right side of the heart, which had been a kind of train wreck that they weren’t even trying to fix yet, was now ejecting blood. Not perfectly; they had some work to do making the atria (the upper chambers of the heart), and the ventricles (the lower chambers), work a little less abruptly to mirror the action of a real heart. But close.
The team would follow up their initial findings on the C90 by refining their model, and began to ask questions about how heart attacks and valve disease would affect proper heart function and how doctors could restore it. In a single step, Mario had gotten them closer to this goal than they’d imagined. They were well on their way to a useful medical tool.
